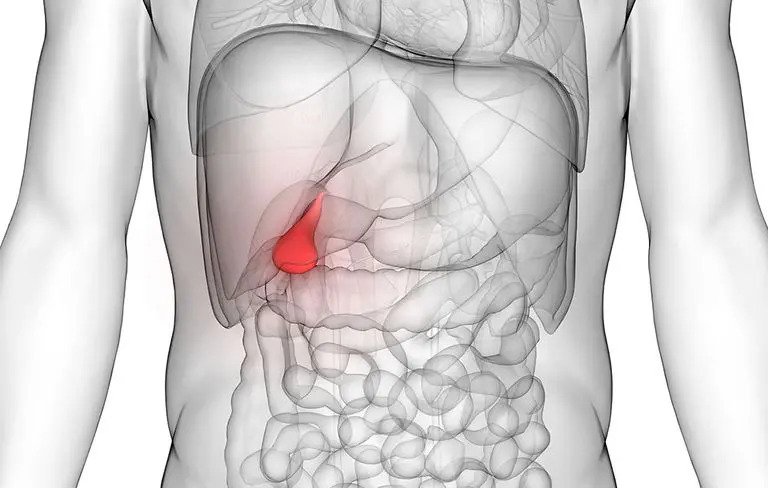
Gallstones are small stones that develop in the gall bladder. The condition is quite common and is also genetic in many cases. The chances of developing gall bladders increase with age. People who eat a fat-rich diet are particularly susceptible to it. The ailment can cause severe symptoms; the most common is returning attacks of shooting abdominal pain.
[Orgirinally Published: http://drmanastripathy.com/laparoscopic-cholecystectomy/]
Treatment:
Gallstones can be dissolved or disintegrated into tiny pieces but these treatments involve the use of drugs with possible side effects. Besides, there is a high rate of failure. In many cases, the gallstones form again. Antibiotics can heal infections of the gall bladder due to the stones. A low-fat diet can also help in preventing pain. However, the alleviation of symptoms is temporary.
Surgery:
Laparoscopic surgery for gallstones or cholecystectomy is a procedure, in which the gall bladder (and gallstones) is removed. After making incisions in the abdomen, the surgeon will inflate the abdomen with carbon dioxide, in order to see the interior more clearly. The surgeon then inserts a telescope, which is attached to a video camera. This will guide him (through a video monitor) while inserting more surgical instruments in the other incisions in order to remove the gall bladder. Before removing the bladder, the surgeon may take a special x-ray (intraoperative cholangiography) to see the locations of the bile ducts inside the liver.
After surgery, the bile will flow from the liver into the small intestine through the common bile duct. Since the gallbladder has been removed, the body will no longer be able to store bile between meals. This has little or absolutely no effect on the process of digestion in the majority of people.
Laparoscopic cholecystectomy is performed under general anesthesia and lasts for 45 minutes to an hour.
Complications:
There may be some complications as with most surgeries. In a few laparoscopic cholecystectomies, the surgeon may switch to open surgery, if a larger incision is required. These can cause additional complications like scars, inflammation, and bleeding. More serious complications may include:
- Development of a hernia at the surgery site
- Injuries to nearby abdominal structures
- Surgical emphysema
- Leaking of bile or leftover stones
- Chronic pain
- Diarrhea
- Bowel injury
- Damage to the liver
- Recovery
Patients are generally discharged the following day. Convalescence may take between two to four weeks depending on the extent of surgery and your type of occupation. Check with the surgeon before the operation about how much you can exercise. For the first few days, increasing how much you walk is recommended. You can expect a full recovery and be able to eat normally during